Common Dental Problems
-
Dental Caries
-
Unfortunately, dental caries (dental decay, 'holes', 'cavities') is common in children (in Australia, 46% of children under age of 6 has dental caries)
-
It is a continue spectrum - early decay looks chalky in colour, to brown cavities
-
The child may or may not report pain
-
It results from a combination of factors (not just from one thing e.g. not brushing the teeth)
-
Dental caries occur when the balance between risks (e.g. frequent consumption of drinks containing sugar like fruit juice, inability to remove plaque - tooth brushing adequately or routinely) and prevention (e.g lack of exposure to fluoride - for example from tap water or use of fluoride toothpaste) is tipped (more risks than prevention)
-
It occurs over time when bacteria in the mouth uses any form of sugar and produce acid, which cause minerals in to be lost from the teeth, causing 'holes'. It usuall gets worse over time.
-
To prevent dental caries, one have to reduce the risks and increase the prevention. Depending on the child, it may or may not be possible to eliminate all risk factors from the diet. If that is the case, then more prevention (e.g. brushing more frequently, higher fluoride concentration toothpaste) will be required. On the other hand, if effective brushing is not possible, then reducing the risks (e.g. less frequent sugar intake) will be beneficial.
-
Dental caries are usually treated by fillings (e.g. tooth-coloured fillings, stainless steel crowns)
-
If the dental caries progress and getting close to the 'nerve' (towards the middle of the tooth), then more comlpex treatment may be required
-
-
Dental abscess / swelling
-
When the dental caries progress (due to inability to maintain the balance towards prevention), it can progress into the 'nerve' (towards the middle of the tooth). Over time, the bacteria will travel down the tooth and cause infection to the tissues around. This can lead to swelling in the gum (abscess), or if more severe, swelling in the cheek or face
-
Dental abscess / swelling in children usually require the offending tooth to be taken out
-
-
Dental erosion
-
Lost of tooth structure due to acids either from the body (for example gastric juice from reflux) or more commonly, from the diet (for example acidic fruits like apples, kiwi fruits, oranges, fruit juice, cordial, soft drinks, energy drinks)
-
-
Periodontal Disease (Gingivitis, Periodontitis)
-
This means the health of the gum and/or the bone around the teeth are not healthy
-
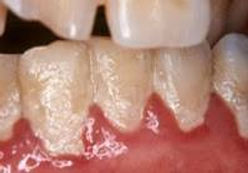
Gingivitis = inflammation of the gum, usually associate with inadequate removal of plaque around the teeth (ie ineffective brushing), the gum react to the presence of the plaque, resulting in the gum being inflammed. The gum usually looks red and swollen and bleeds easily during brushing or flossing
-
Gingivitis has been reported to be more severe in children with ASD as tooth brushing could be quite challenging. We have many suggestions to help with tooth brushing here for you to consider
-
Periodontitis = infection of the bone supporting the teeth resulting from bacteria present around the gum or the teeth - uncommon in children (unless medically compromised e.g. immune deficiency)
-
-
Dental Trauma
-
Dental trauma is common in children, but some studies reporting that it is even more common with children with ASD
-
Trauma to teeth is never the end of the world so the most important thing is to keep calm
-
Contact your dentist and discuss what had happened and for assessment
-
Complicated trauma to the teeth sometimes require management by a specialist or at a hospital setting
-
Common Dental Procedures
-
Check-up
-
Dental examination - checking the health of all oral structures, identify any problems, discuss ways to improve oral health. Pictures of some of the instruments used by the dentist can be found under visual aids
-
-
X-rays
-
X-rays are usually needed to check between the teeth for dental caries (that cannot be visualised by looking in the mouth as the teeth can be very tight together at the back), or for checking the presence and location of adult teeth in children, or to assess presence of any infection or pathology
-
-
Clean
-
Professional clean usually involves using special instruments to remove calculus (tartar) build-up as the build-up (which is usually yellow and hard that stuck to the teeth) cannot be removed by normal brushing alone. It also involves thorough removal of plaque (sticky white/yellow film on the teeth near the gum) build-up with an electric-powered instrument
-
-
Fluoride application
-
Fluoride of higher concentration (compared with toothpaste) in form of gel, foam, or vanish is usually used in the dental clinic. Studies shown that professional application of fluoride at least twice a year can reduce dental caries significantly
-
-
Dental restorations (fillings)
-
Involves removal of the weakened tooth structure including the bacteria (removing all the 'brown' decay) and restoring that missing portion of the tooth (usually with a white filling if the hole is small, or a stainless steel crown if the hole is larger for the back baby molar teeth where a white filling may not be strong enough)
-
-
Dental extractions
-
Involve numbing up the tooth and removing the tooth
-
-
Space maintainers
-
In some cases, if a baby tooth (usually at the back) is removed earlier than when the adult tooth underneath is suppose to come through, the teeth nextdoor may move into the space, and the adult tooth underneath would not have enough space to come through. Space maintainers (usually in form of a metal band and wire loop), can help to keep that space there following removal of a baby tooth
-
-
Fissure sealants
-
These are coatings that can be placed to seal up the pits and grooves on the eating surfaces of the molar (back) teeth, where bacteria can hide and cause problems. Studies shown that fissure sealants are very effective in preventing dental caries from forming in adult molar teeth
-









Orthodontic Treatment
-
Usually carried out by orthodontists
-
Plates
-
Braces
-
In many cases, orthodontic treatment is possible. Some modifications can be catered to individual needs
Where to go?
Who else can help?
-
Occupational Therapists
-
-
Psychologists
-
Speech Pathologist
-
Paediatrician
-
Family and friends
-
Other parents
General Anaesthesia
For some dental treatment, it may be easier and safer to be performed under a general anaesthetic procedure. This is usually carried out in a public or private hospital as a day-procedure (can go home on the same day). All Paediatric Dentists (Children's Dentists) and some general dentists offer dental treatment under general anaesthesia. A premediation may be given to help settle the child prior to the general anaesthetic procedure, depending on the anaesthetist recommendation.
Relative Anaesthesia
Relative anaesthesia (Nitroux oxide sedation/inhalation sedation/Happy Gas) could be a suitable option for dental procedures. It involves the child wearing a mask (can place fruity flavourings) on the nose. It is a very safe option and helps keep the child relax. However, not all children are suitable to have dental procedures done under relative anaesthesia. If the child is not able to keep the mask on, or is extremely nervous or distressed, relative anaesthesia would not be effective.
